The agony of hives
03/15/2017
For some, hives are an existence of chronic irritation. They present randomly, burn, sting and campaign to ruin your day with constant reminder.
For those lucky not to have experienced them yet doesn’t mean you won’t. There is a 15% chance you could get hives at least once in your lifetime (girls, your chances are higher than boys (1) ) even if it’s just ‘acutely’; defined as less than 6 weeks duration.
Although 1.8% of adults worldwide battle with them regularly, right now! (2)
A real b-*–itch.
People absolutely hate them and they give people real anxiety. Hive sufferers having higher rates of psychological distress (3) The physical discomfort compounded by the emotional torture that there is no cure to end the wretched affliction rates them high on A-n-n-o-y-i-n-g.
Chances are there would be many chronic hive sufferers out there who remain frustrated with diagnosis; or lack of diagnoses. Even if they saw their local doctor about it; the front-line primary response that
“Hives are rarely due to a nasty underlying disease. Although they can be uncomfortable and cosmetically embarrassing, they are not dangerous. Most people with hives do not need tests” (ASCIA, Urticaria)
can be somewhat deflating if your living with chronic hives.
Not nasty. Not dangerous. No tests recommended.
Left to manage urticaria chronically or left on long waits to see one of the highest privately billing specialists (4)- making access to allergy specialty care hard, if you want you to find out more about the unremitting itch.
Hence the WAO 2017 theme “The Agony of hives”.
To top it off, even if you see an allergist, allergy testing often yields no answers (5) making idiopathic chronic urticaria a frustratingly common diagnosis ie. no cause identified.
It’s hard to swallow but in 80% of cases, a cause is not identified.
Although an autoimmune basis of most of the ‘idiopathic’ forms is now being hypothesised. (6,7)
Said differently, because urticaria can be caused by absolutely almost anything (the list of causes as long as your arm) it’s often hard to work it out, especially on your own. It takes real medical detective work and a good physician ready to outshine the failings of “google-medicine” by showcasing how careful history-taking is actually the best form of assessment.(5)
During a typical chronic urticaria consultation, much time is spent breaking down popular misled beliefs. At the front line of primary care allergy medicine, 2017 World Allergy Week is an opportunity to shatter 3 current common hives misconception.
1. Hives = Allergy
2. Patients with hives need allergy skin prick testing.
3. There is nothing much anyone can do about hives
1. Hives = allergy
While it is true that Allergies can cause hives, the reverse is not, hives are not only always caused by allergies.
Hives can be caused by so many things – from changes in temperature, cold weather or infections to preservatives and common medications like codeine, aspirin or even oral contraceptive pills.
A #PractitionersPearl is to always check their medication history.
Medications are infact a common cause of chronic urticaria commonly overlooked because of this following fact.
Medications can still cause hives even if you have been on them for a while….making diagnoses tricky because patients least expect it to be their blood pressure table, oral contraceptive pill , NSAID or aspirin.
A pearl for patients out there is not to overlook an obvious immeasurable cause of hives – stress. Classically hives can be the tell-tale sign of stress
Its refreshing to see actors like Anne Hathaway readily admit to being afflicted with urticaria when they are nervous, bothered or hot under the collar.
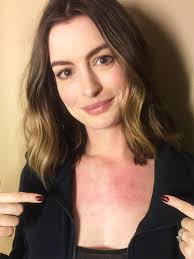
2. Patients with hives need allergy skin prick testing.
Many patients seen at our collective. care allergy and Australian Allergy Centre clinics regarding chronic hives expect skin pick testing to confirm their suspicion that their hives are caused by food or an environmental allergens. Not true.
In fact, the role of allergy skin prick testing is controversial in the investigation of chronic urticaria. Food allergy actually represents such a small possible cause many argue about the value and many test results are not always clinically useful, therefore skin prick testing is reserved for when the history is suggestive of an allergic cause.(5)
Other tests outside of allergy testing like inflammatory blood markers (ESR), thyroid function + antibodies, autoimmune screens, coeliac testing as well as skin biopsies (if there is concern of urticaria vasculitis) are sometime arranged to filter through the list of possible underlying causes.(8)
3. There is nothing anyone can do about hives
While there is no cure there still are treatments. Although time is truly the wonder healer with 80% of urticaria settling within 12 months. (9) But when a cause isn’t immediately obvious, patients face trialling different measures or medications to control the symptoms of urticaria.
First line treatment currently involves reassurance, avoidance of exacerbating factors and non-sedating antihistamines. (10) Traditional antihistamines, if not working at usual doses can be prescribed up to 4 times the labelled dose to help achieve adequate control. Additionally the use of H1 and H2 receptor antagonists such as doxepin can be titrated up balancing against side effects like sedation. (11)
There is some light at the end of the tunnel with newer modalities.
While narrow band UV-B phototherapy treatment still remains inconclusive although with some promising results as an alternative treatment (12), immunodulator, omalizumab injections currently approved for asthma, is showing really promising results. The World Allergy Organisation Journal quotes (13, 14, 15) large multi centre, randomised, double-blind, placebo controlled phase III trials of omalizumab, at doses of 150 and 300mg every 4 weeks for 3 months show significantly improved urticaria outcomes compared with placebo.
…….. it’s currently awaiting PBS listing in Australia-Otherwise this treatment costs over $400 per shot – chronic urticaria sufferers, let’s hope it’s not another agonising wait.
More radical therapy in the form of immunoglobulins, plasmapheresis and cyclophosphamide are being used for recalcitrant cases. Autologous transfusion and alternative remedies like acupuncture have prospects for future too.
Other therapies including psychological treatments and acupuncture should be offered. In one study acupuncture induced partial remission of chronic urticaria in the majority of the patients. During 3 weeks of study, the efficacy of acupuncture was greatest in the third week of treatment (16) and many studies (17,18,19) suggest psychological treatments such as relaxation treatments and hypnosis positive impact for urticaria.
What collective.care Allergy Clinic plans to contribute for this 2017 The Agony of Hives World Allergy Week
At collective.care allergy our commitment to health professionals and community education includes:
A well-overdue explanation about the complexity of chronic hives to the public
Acknowledgment of their relentless nature and effect of psychological health
Acknowledgement of the difficulty in identifying a cause for chronic urticaria
Commitment to continue to send updates to our patients about any new emerging treatments that become available including PBS listing of Omalizumab
Pioneer our collective.care chronic urticaria case conferencing so we can collaboratively manage with allergy, immunology, dermatology, general practice, acupuncture and psychologists chronic urticaria using chronic disease management planning principles.
———————————————————————————————————-
About:
Dr Suzan Bekir MBBS (Hons1) FRACGP is co-creator of collective.care and Australian Allergy Centre, Australia’s first GP-shared care model for specialist clinics including Allergy, ENT, skin, laser and cosmetic medicine. She is clinical director and head of GP accredited special skills training programs for Allergy, ENT, eye, metabolic, skin, laser and cosmetic medicine.
For any Media enquiries for upcoming World Allergy Week 2017 please contact Christian Burden on 0481940809.
References :
Deacock SJ. An approach to the patient with urticaria. Clin Exp Immunol. 2008;153:151–61.
Zuberbier T, Balke M, Worm M, Edenharter G, Maurer M. Epidemiology of Urticaria; a representive cross-sectional population survey. Clin Exp Dermatol 2010; 869-73.
3. Ozkan M, et al.Psychiatric morbidity and quality of life in patients with chronic idiopathic urticaria. Ann Allergy Asthma Immunol. 2007.
4. Gary L Freed and Amy R Allen. Variation in outpatient consultant physician fees in Australia by specialty and state and territory. Med J Aust 2017; 206 (4): 176-180.
5. S Fernando et al. Chronic urticaria. Assessment and treatment. Australian family physician. Vol 39 (3):2010
6. Sharma VK, Gera V, Tiwari VD. Chronic urticaria: Expanding the autoimmune kaleidoscope. Med J Armed Force India. 2004; 60:372-8.
7. Dalal I, Levine A, Somekh E, Mizrahi A, Hanukoglu Chronic urticaria in children: Expanding the “Autoimmune Kaleidoscope” Pediatrics. 2000;106:1139–41.
8. Wai YC, Gordon LS. Evaluating chronic urticaria patients for allergies, infections, or autoimmune disorders. Clin Rev Allergy Immunol. 2002;23:185
9. Gaig P, Olona M, Munoz Lejarazu D, et al. Epidemiology of urticaria in Spain. J Investig Alergol Clin Immunol, 2004; 14:214-20.
10. ASCIA. urticaria. https://www.allergy.org.au/images/pcc/ASCIA_PCC_Urticaria_hives_Feb2017.pdf
11. Smith P, Corelli R .Doxepin in the management of pruritus associated with allergic cutaneous reactions. Ann Pharmacother 1997;31:633–5.
12. Aydogan K metal. Narrowband UVB (311nm, T1L01) phototherapy in chronic urticaria. International Journal of Dermatology. Jan 2012 (51)1:98-103.
13. Maurer M, Rosén K, Hsieh H-J, Saini S, Grattan C, Gimenéz-Arnau A, et al. Omalizumab for the treatment of chronic idiopathic or spontaneous urticaria. N Engl J Med [Internet]. Massachusetts Medical Society; 2013 [cited 2016 Apr 8];368(10):924–35.
14. Saini SS, Bindslev-Jensen C, Maurer M, Grob J-J, Bülbül Baskan E, Bradley MS, et al. Efficacy and safety of omalizumab in patients with chronic idiopathic/spontaneous urticaria who remain symptomatic on H1 antihistamines: a randomized, placebo-controlled study. J Invest Dermatol [Internet]. 2015 [cited 2016 Apr 5];135(1):67–75.
15. Kaplan A, Ledford D, Ashby M, Canvin J, Zazzali JL, Conner E, et al. Omalizumab in patients with symptomatic chronic idiopathic/spontaneous urticaria despite standard combination therapy. J Allergy Clin Immunol. 2013;132(1):101–9.
16. Iraji F, Saghayi M, Mokhtari H, Siadat A. The efficacy of acupuncture in the patients with chronic urticaria: Acupuncture in the treatment of chronic urticaria: A double blind study. Int J Dermatol. 2006;3:2.3:185
17. Buffet M et al. Management of psychological factors in chronic urticaria. When and how. Ann Dermal Venereol 2003.
18. Bering AM et all. Chronic urticaria: importance of medical-psycological approach. Our Ann Allergy Clin Immune, 2006.
19.Consoli SG wet al. Psychological factors in chronic urticaria. Ann Dermal Venereol. 2003.